Background
Dental Implant surgery is a common procedure in modern dentistry that has been used for over 40 years. It allows artificial teeth to be implanted firmly in jaw bones, and techniques vary from replacing one missing tooth to replacing most teeth in the upper and/or lower jaw. Dental implants are just one solution to replacing teeth that have been extracted or failed to develop. Implant treatment is performed within a team environment consisting of your dentist, oral surgeon, hygienist, and most importantly the patient. Treatment is rarely successful without this teamwork mindset.
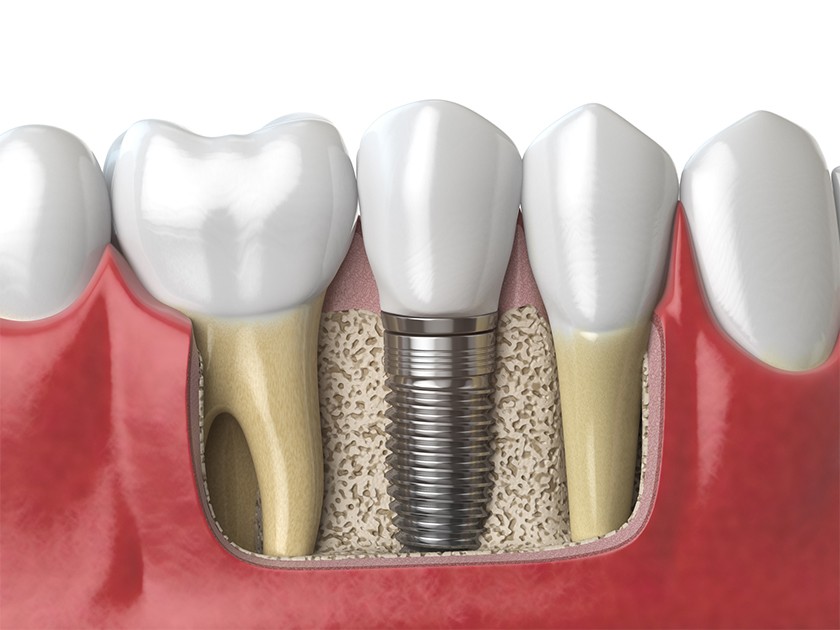
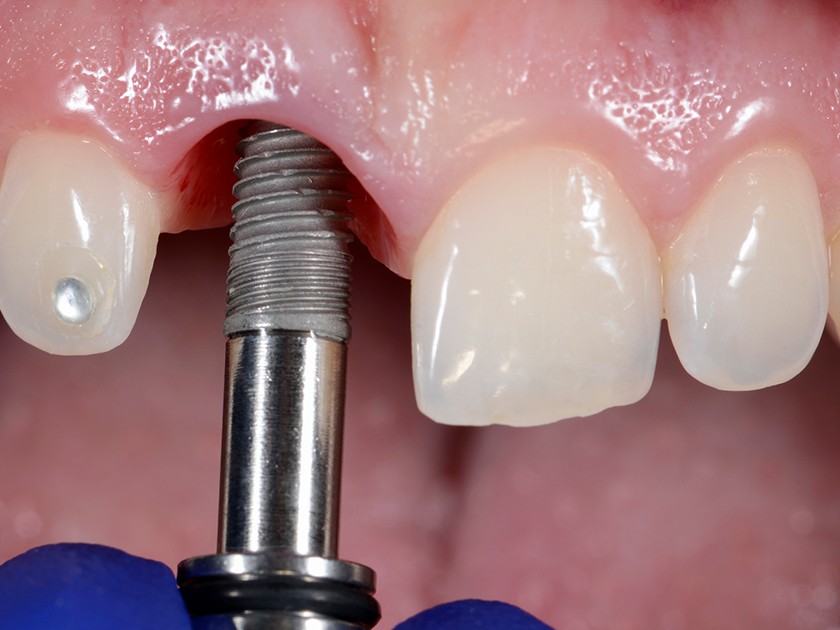
Components of a Dental Implant
Implant Fixture: A titanium implant fixture is inserted into the jaw bone to provide a solid foundation to support and attach the prosthesis.
Prosthesis: This is an artificial tooth, or row of artificial teeth, attached to the implant fixture. Some prostheses can be removed for daily cleaning (e.g. an overdenture), and others are fixed to the underlying implant.
The prosthesis can be:
- Crown - to replace one missing tooth
- Bridge - to replace several missing teeth
- Denture - to replace a full dental arch
Advantages of Dental Implants
Implants help to solve problems posed by traditional dentures and bridges. They can provide points of firm attachment for dental prostheses and can have the following advantages :
- Dental implants can be more comfortable, convenient and attractive than the dentures
- Fewer problems when eating and talking than dentures
- Biting and chewing are similar to normal teeth
- Bridges require healthy teeth to be cut and reshaped to fit the bridge in place
- Natural teeth do not have to be altered or damaged when dental implants are used
Biology of Implants
Implants are made of biocompatible materials (e.g. titanium) which can bond strongly to bone as it grows onto the implant’s surface by a process called osseointegration. Once healed, this forms a firm base to allow the implant and bone to withstand the daily forces of chewing and normal function.
When to have Dental Implants?
Dental implants can be placed after the age of 16 or 17 once bone growth has mostly stopped. Most adults can have dental implants placed at any age, however a thorough examination and assessment by your Oral Surgeon will be needed to ensure there are no underlying conditions that will affect your surgery or the success of the dental implant.
Following the referral from your dentist, your assessment will include:
- A consultation appointment consisting of a thorough history and
- Imaging : this is a low dose scan called a cone beam CT scan (CBCT) that allows assessment of the jaw bones and to simulate the surgery
- Impressions and models of your teeth
- Photography to aid in the planning of surgery
You are encouraged to take an active role in your implant therapy and the making of decisions. The decision to have implants is always yours, so do not be pressured by anyone. Dr Singh and your dentist will be happy to answer any questions your may have.
A realistic outlook is important as implant therapy is not successful for everyone. All types of medical and dental treatments have complications, and some reconstructions can be very difficult; the results may not be as good as hoped.
Some medical conditions and medications preclude the placement of implants, so having a medically qualified surgeon is important. An example is the use of bisphosphonates which are often used to treat osteoporosis and other bone conditions, and work by decreasing bone turnover. In these circumstances implants may fail to integrate or later may lose integration. The risk is low with oral bisphosphonates (about 1%) but high with intravenous bisphosphonates (about 15%).
Bone grafts and regeneration
In some patients, bone grafts are required to provide extra bone to provide a secure base for the implants. The bone is usually taken from another part of the jaw or from the hip. In addition guided-tissue regeneration can be used to augment the bone stock prior to, or during, implant placement.
Smoking
Smoking can cause the bone to implant bond to fail and thus significantly increase the risk of failure. Many surgeons will not place implants in these circumstance so it is best to quit prior to considering dental implants.
Options for Implant placement
Once you have been fully assessed and a treatment plan formulated, your dental implant surgery can take place in a variety of settings appropriate for you. This includes under surgery under local anaesthetic only, conscious sedation, or general anaesthetic in a day procedure hospital or clinic. Care will be individualised to you and your circumstances after a full and open discussion about your treatment options.
Procedure
Once you are appropriately anaethetised, your surgeon will make an incision in your gums to expose the underlying bone. A number of precision drills will be used to prepare the site prior to the implant being inserted into the jaw bones in a planned manner. Sometimes a guide or splint is used to ensure the implant is placed into the correct area. Occasionally bone graft materials are used to help with bone healing. The whole area is cleaned thoroughly and often a healing abutment/cap is placed and the gums are then stitched around this using dissolvable stitches (Single Stage Procedure). The bone around the implant is then allowed to heal for a period of 3-6 months prior to construction of a permanent prostheses, however in the interim your dentist or prosthodontist will place a temporary prostheses if the situation is appropriate. Sometimes the gums are closed over the implant completely, and the abutment is placed at a later date with a small surgical procedure under local anaesthetic (Second Stage Procedure).
Oral Hygiene
Meticulous oral hygiene of the implant site, teeth, gums, and prostheses is crucial to improve the chances of success in the short and long term. Implant hygiene is a life-time commitment for the patient and dentist, and if your mouth needs periodontal care it should be carried out in a regular and timely manner with your dentist or hygienist.
Success Rates
There are a variety of factors that will influence the success of implants over time. These include:
- Your general health including smoking, nutritional status
- Your periodontal (gum) health and oral hygiene
- The health of the jaw bone and its ability to heal
- The type of dental implant
- The type of prosthesis and the number of implants used
- Where the implant is placed in your mouth (e.g. Upper vs Lower Jaw)
- The skill and experience of your surgeon
According to international literature approximately 95 patients in every 100 can expect to have successful treatment, with 9 out of 10 implants remaining in place for 10 – 20 years or more. However, each situation is different and thus it is difficult to predict how long an implant will function in an individual.
After Care
Following the anaesthesia and placement of your dental implant(s), you can usually make a safe and comfortable recovery at home with your family or friends once you are discharged from the clinic or hospital.
Normally a prescription will be given to you for pain killers, antiseptic mouthwash, anti-inflammatories, and usually antibiotics. This will be discussed with you prior to surgery so ensure you are comfortable with the medications prescribed.
To aid a comfortable recovery please make sure you:
- Rest at home after the surgery
- Do not drive, engage in active exercise or sports, or operate machinery
- Take several days off school, work, or other duties
- Keep the areas clean with mouthwashes and gentle toothbrushing
- Do not drink alcohol while taking your medications
- Do not smoke
- Use ice packs to reduce pain and swelling in the first 48 hours
- Have a soft meals
Follow-Up
A follow-up appointment is usually scheduled for 1-2 weeks following the placement of your dental implant to assess healing and progress. If you are unable to attend your follow-up appointment, then please call the clinic to reschedule or cancel your appointment.
If you would like to schedule an appointment with Dr. Singh to discuss dental implants then please contact us here.